Neurons in Anterior Gray Horn
The neurons of the anterior gray horn are involved in motor function and send motor nerve fibers to muscles and other effector organs.
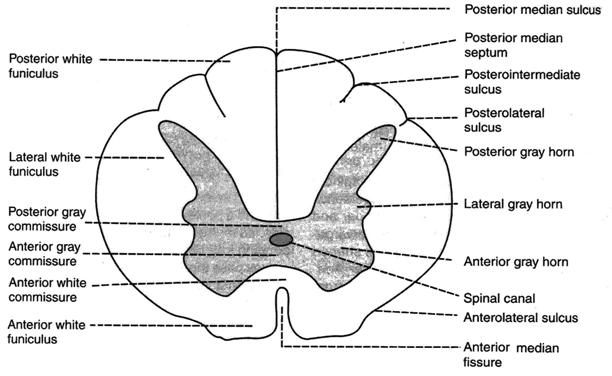
Fig.18.Section of spinal cord — thoracic segment.
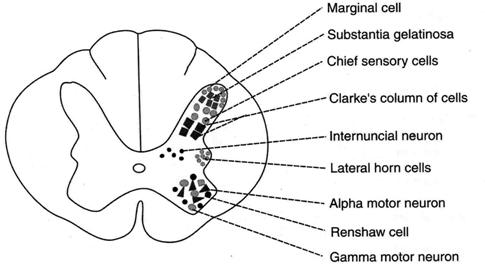
Fig.19.Neurons in gray horn of spinal cord — thoracic segment.
Three types of motorneurons are located in anterior gray horn.
Alpha motorneurons: Alpha motor neurons are large and multipolar cells. Axons of these neurons leave the spinal cord through the anterior root and end in groups of skeletal muscle fibers, i.e. extrafusal fibers.
Gamma motor neurons: Gamma motor neurons are smaller cells scattered among alpha motor neurons. These neurons send axons to the intrafusal fibers of the muscle spindle.
Renshaw cells: These cells are also smaller cells. Renshaw cells are the inhibitory neurons playing an important role in synaptic inhibition at the spinal cord.
Neurons in Lateral Gray Horn
in thoracic and upper two lumbar segments, the gray matter forms a small projection in between the anterior and posterior horns. This is called the lateral gray horn. This has cluster of nerve cells called intermediolateral horn cells. These cells give rise to sympathetic preganglionic fibers, which leave the spinal cord through the anterior nerve root.
Neurons in Posterior Gray Horn
The posterior gray horn contains the sensory neurons, which receive impulses from various receptors of the body through posterior nerve root fibers. Four groups of neurons are present in the posterior gray horn.
Substantia gelatinosa of Rolando: This is a cap like gelatinous material at the apex of posterior horn. This is formed by smaller nerve cells.
Marginal cells: Marginal cells cover the substantia gelatinosa at the very tip of the posterior gray horn. Sometimes the marginal cells are also called the border cells.
Chief sensory cells: The chief sensory neurons are situated in the remaining parts of posterior column.
Clarke's column of cells: The Clarke's column of cells is the collection of well-defined cells and occupies the inner part of posterior horn.
WHITE MATTER OF SPINAL CORD
White matter of spinal cord surrounds the gray matter. It is formed by the bundles of both myelinated and non-myelinated fibers, but predominantly the myelinated fibers. The anterior median fissure and the posterior median septum divide the entire mass of white matter into two lateral halves. The band of white matter lying in front of anterior gray commissure is called the anterior white commissure.
|
|
|
Each half of the white matter is divided by the fibers of anterior and posterior nerve roots into three white columns or funiculi.
1. Anterior or Ventral White Funiculus
This lies between the anterior median fissure on one side and anterior nerve root and anterior gray horn on the other side.
2. Lateral White Funiculus
This is present between the anterior nerve root and anterior gray horn on one side and posterior nerve root and posterior gray horn on the other side.
3. Posterior or Dorsal White Funiculus
It is situated between the posterior nerve root and posterior gray horn on one side and posterior median septum on the other side.
Spinal proper functions:
1. Spinal reflexes.
2. Organism motor activity co-ordination particularly spinal motoneurons functions.
3. Vegetative reactions.
4. Uroreleasing and defecation.
Spinal animals – are animals with cutted spine on the boarder with medulla oblongata.
Spinal animals features:
1. Respiration absence.
2. Low blood pressure, decreased vascular tone.
3. Loosing the ability to support homoiothermism (constant body temperature).
4. Disapperance of all forms of singleminded activity (alimentary, sexual, protective).
5. Anal and uroreleasing ceneters paralysis at spine cutting lower than lumbal parts.
Spine vegetative functions:
1. Defecation.
2. Uroreleasing.
3. Vascular tone regulation.
4. Erection and ejaculation.
5. Sweat releasing.
Spine afferent ways:
1. Goll’s and Burdah’s ways.
2. Spinal-thalamic tracts.
3. Spinal-cerebellar tracts.
Significance of afferent information coming into spine:
1. It carries the information about environment changings.
2. It participates in CNS co-ordinative activity by guiding the skeletal musculature: at switching-off the afferent impulsation from working organ its guiding becomes non-perfect.
3. It encourages CNS tone supporting; summary tonic CNS impulsation is decreased at afferent impulsation switching off.
4. It participates in inner (visceral) organs regulation processes.
Efferent ways:
1. Pyramidal tract.
|
|
|
2. Extrapyramidal ways:
A) reticulo-spinal tract;
B) rubro-spinal tract;
C) tecto-spinal tract;
D) vestibule-spinal tract.
PYRAMIDAL TRACTS
Pyramidal tracts of spinal cord are descending tracts concerned with voluntary motor activities of the body. These tracts are otherwise known as corticospinal tracts. There are two corticospinal tracts, the anterior corticospinal tract and lateral corticospinal tract. While running from cerebral cortex towards spinal cord, the fibers of these two tracts give the appearance of a pyramid on the upper part of anterior surface of medulla oblongata. Hence, these two tracts are called pyramidal tracts.
The pyramidal tracts are concerned with voluntary motor activities and were the first tracts to be found in man (Fig. 20).

Fig. 20. Corticospinal tract.
Nerve fibers of pyramidal tracts: All the fibers of the pyramidal tracts are present since birth. However, the myelination of these fibers is completed in about two years after birth. The pyramidal tracts on each side have more than a million fibers. About 70% of the fibers are myelinated and large having a diameter of 4 to 22 microns.
Larger fibers of pyramidal tracts have the tendency to disappear at old age. Since these tracts are concerned with control of voluntary movements, the disappearance of the fibers of pyramidal tracts causes automatic shivering movements in old age.
The fibers of pyramidal tracts are the axons of upper motor neurons.
Origin
Fibers of pyramidal tracts arise from the following nerve cells in the cerebral cortex.
1. Giant cells or Betz cells or pyramidal cells in precentral gyrus of the motor cortex. The giant cells are situated in area 4 (primary motor area) of frontal lobe of the cerebral cortex.
2. Other areas of motor cortex namely, premotor area (area 6) and supplementary motor areas.
3. Other parts of frontal lobe.
4. Parietal lobe of cerebral cortex particularly from somatosensory areas (areas 3,1,2). It is believed that 30% of pyramidal fibers arise from primary motor area (area 4) and supplementary motor areas, another 30% from premotor area (area 6) and the remaining 40% of fibers arise from the parietal lobe particularly from somatosensory areas (areas 3,1,2). All the above fibers form the fibers of upper motor neurons of motor pathway.
|
|
|
Course
After taking origin, the nerve fibers run downwards in a diffused manner through white matter of cerebral hemisphere and converge in the form of a fan like structure along with ascending fibers which project from thalamus to cerebral cortex. The fan like structure is called corona radiata. Then, the fibers descend down through internal capsule, midbrain and pons. While descending through pons, the fibers are divided into different bundles by the nuclei of pons. At the lower border of pons, the fibers are grouped once again into a compact bundle and then descend down into medulla oblongata.
This compact bundle of corticospinal fibers gives the appearance of a pyramid in the anterior surface of upper part of medulla. Because of this, the corticospinal tracts are called the pyramidal tracts.
At the lower border of medulla, the pyramidal tract on each side is divided into two bundles of unequal sizes. About 80% of fibers from each side cross to the opposite side. Thus, the fibers of both sides while crossing the midline form pyramidal decussation. After crossing and forming pyramidal decussation, the fibers descend through the posterior part of lateral white funiculus of the spinal cord. This bundle of crossed fibers is called the crossed pyramidal tract or lateral corticospinal tract or indirect corticospinal tract.
The remaining 20% of fibers do not cross to the opposite side but descend down through the anterior white funiculus of the spinal cord. This bundle of uncrossed fibers is called the uncrossed pyramidal tract or anterior corticospinal tract or direct corticospinal tract. This tract is well-marked in cervical region. Since, the fibers of this tract terminate in different segments of spinal cord, this tract usually gets thinner while descending through the successive segments of spinal cord. The fibers of this tract are absent mostly below the midle thoracic level. Before termination, majority of the fibers cross to the opposite side at different levels of spinal cord.
|
|
|
Termination
All the fibers of pyramidal tracts, either crossed or uncrossed, terminate in the motor neurons situated in anterior gray horn either directly or through internuncial neurons. The axons of the anterior motor neurons supply the skeletal muscles directly by passing through the anterior nerve root. The neurons giving origin to the fibers of pyramidal tract and their axons are together called the upper motor neurons. The anterior motor neurons in the spinal cord and their axons are called the lower motor neurons.
Function
The pyramidal tracts are concerned with voluntary movements of the body. Fibers of the pyramidal tracts transmit motor impulses from motor area of cerebral cortex to the anterior motor neurons of the spinal cord. These two tracts are responsible for fine, skilled movements.
Effects of Lesion
The lesion in the neurons of motor cortex and the fibers of pyramidal tracts is called the upper motor neuron lesion. The following are the symptoms:
1) Voluntary movements: Voluntary movements of the body are very much affected. Initially, there is loss of voluntary movements in the extremities. Later, it involves the other parts of the body like hip and shoulder.
2) Muscle tone. The muscle tone is increased leading to spasticity of muscles. The muscles are paralyzed. This type of paralysis of muscles is called the spastic paralysis. The spasticity is due to the failure of inhibitory impulses from cerebral cortex to reach the spinal cord.
3) Reflexes: All the superficial reflexes are lost. And the deep reflexes are exaggerated. Some pathological reflexes are positive.
Дата добавления: 2018-02-15; просмотров: 6792; Мы поможем в написании вашей работы! |

Мы поможем в написании ваших работ!
